Welcome back to Healthy Innovations! 👋
Last week, it was reported that a surgeon in London removed a patient’s prostate while the patient lay in a hospital in Gibraltar – 2,400 km (1,500 miles) away. The entire operation ran with just a 60-millisecond delay, and it worked flawlessly.
I previously covered the rise of robotic surgery in Healthy Innovations:
In this issue, I want to explore what this kind of “surgery without borders” could mean for the billions of people worldwide who cannot access a specialist surgeon.
Let’s dive in.
What is telesurgery?
Telesurgery allows a surgeon to operate on a patient in a completely different location using a robotic system. The surgeon sits at a console and controls the robot's arms in real time. The robot performs the physical procedure at the patient's end.
It's different from telemedicine (video consultations) in one critical way: the surgeon is actually doing the surgery. The robot is the instrument.
For this to work safely, three things need to be in place:
A surgical robot at the patient's location, with a local clinical team to monitor
Ultra-low-latency connectivity — research suggests that keeping round-trip delay below about 200 milliseconds is widely recommended for safe telesurgery
A remote console for the surgeon, which can be located anywhere with a stable high-speed connection.
The Gibraltar procedure ran at 60 milliseconds, faster than a human blink. It used the Toumai Robotic System by MicroPort, connected via fiber optic cable with a 5G backup. A local team was in the operating room throughout, ready to take over if the connection dropped. It didn't.
Why now?
Telesurgery isn't a new idea. In 2001, French surgeon Dr. Jacques Marescaux removed a patient's gallbladder in Strasbourg, France while operating from New York. The procedure worked, but the telecommunications technology of the time made it too expensive and fragile to repeat.
Two decades of progress have changed the picture:
5G networks offer the low latency and high bandwidth that telesurgery requires
Fiber optic infrastructure now spans continents, enabling dedicated high-speed surgical connections
Robotic platforms have become smaller, more reliable, and in some cases more affordable
Regulatory frameworks are starting to catch up, with the first FDA-approved transcontinental telesurgery trial completed in 2025.
That last point is significant.
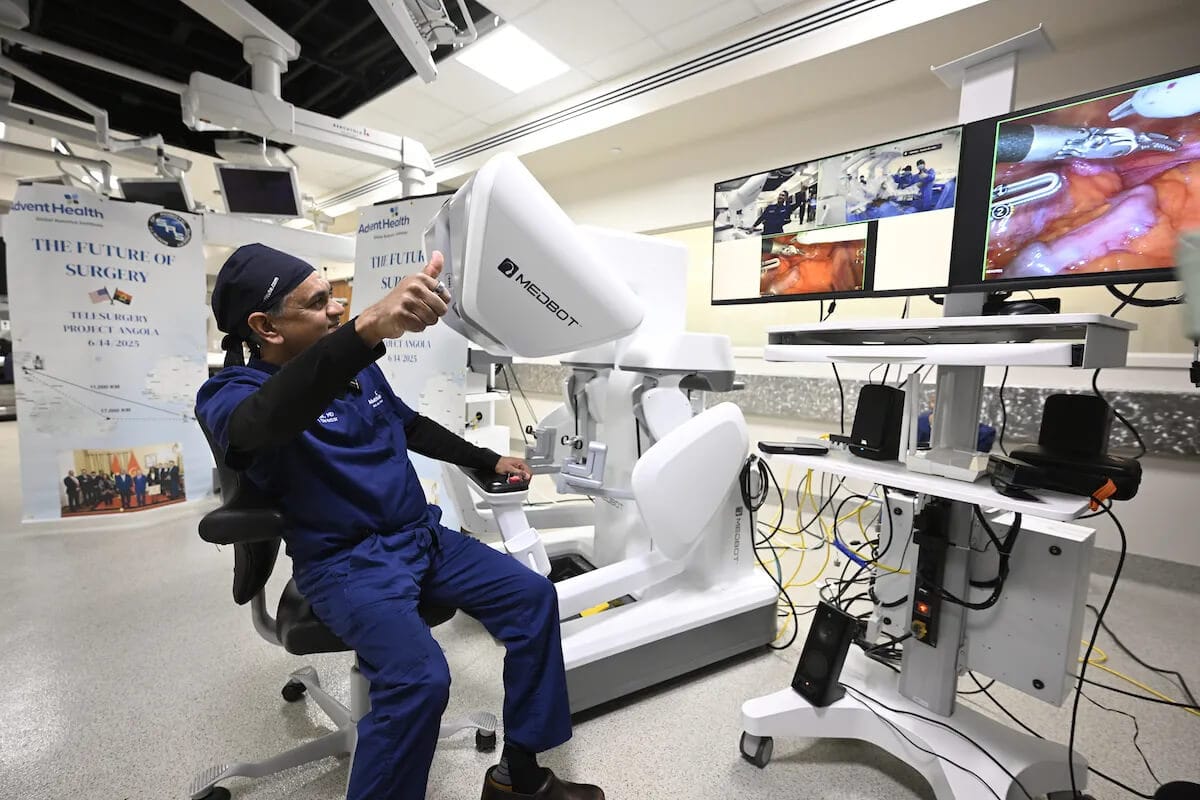
In June 2025, Dr. Vipul Patel at AdventHealth in Florida performed a robotic prostatectomy on a patient in Luanda, Angola, nearly 7,000 miles away, as part of the first FDA-approved IDE human clinical trial of transcontinental telesurgery initiated from the United States. The signal traveled thousands of miles of fiber optic cable on a multi-leg route from Florida to Angola. The patient did well, and AdventHealth planned 10 cases in the trial, several of which have now been completed.
The access problem telesurgery could solve
Surgical expertise is not distributed anywhere close to evenly.
In many low-income countries, there are fewer than one trained surgeon per 100,000 people, and while low-income and lower-middle-income countries represent 48% of the global population, they hold just 19% of the world’s surgeons. The result is staggering: an estimated 5 billion people still lack access to safe, timely surgical care. Meanwhile, the US has historically accounted for the majority of global robotic surgical volume, with some estimates putting its share at around 70% of all cases as recently as 2020.
That imbalance has real consequences.
Angola, where the 2025 FDA trial took place, has one of the highest prostate cancer mortality rates in sub-Saharan Africa, largely because patients cannot access the specialist surgical care that would catch and treat it early. The telesurgery trial was paired with a national prostate cancer screening initiative, also established by Dr. Patel’s team. Screening finds the cancers; telesurgery treats them.
And the access gap is not only international. Rural hospitals across the US, UK, and Europe routinely lack neurosurgery, urology, and oncology specialists, forcing patients to travel long distances for complex procedures, or to go without them entirely.
Who's building it
Several robotic platforms are now actively being used or developed for telesurgery:
MicroPort Toumai (China) — the most proven telesurgical platform, with over 100 human procedures documented at distances up to 5,000 km. Used in urological, hepatobiliary, thoracic, and gynecological surgeries.
SSi Mantra 3 (SS Innovations, India) — achieved the world’s first intercontinental robotic cardiac telesurgery in 2025 (atrial septal defect closure between France and India, over 4,000 miles). Also applied in urology, general, and gynecologic surgery.
Intuitive Surgical da Vinci (US) — the dominant global robotic surgery system, used in telesurgical research and feasibility studies for urologic, gynecologic, colorectal, and thoracic operations.
CMR Surgical Versius (UK) — compact and modular system evaluated for telerobotic general and gynecologic procedures in low‑latency network trials.
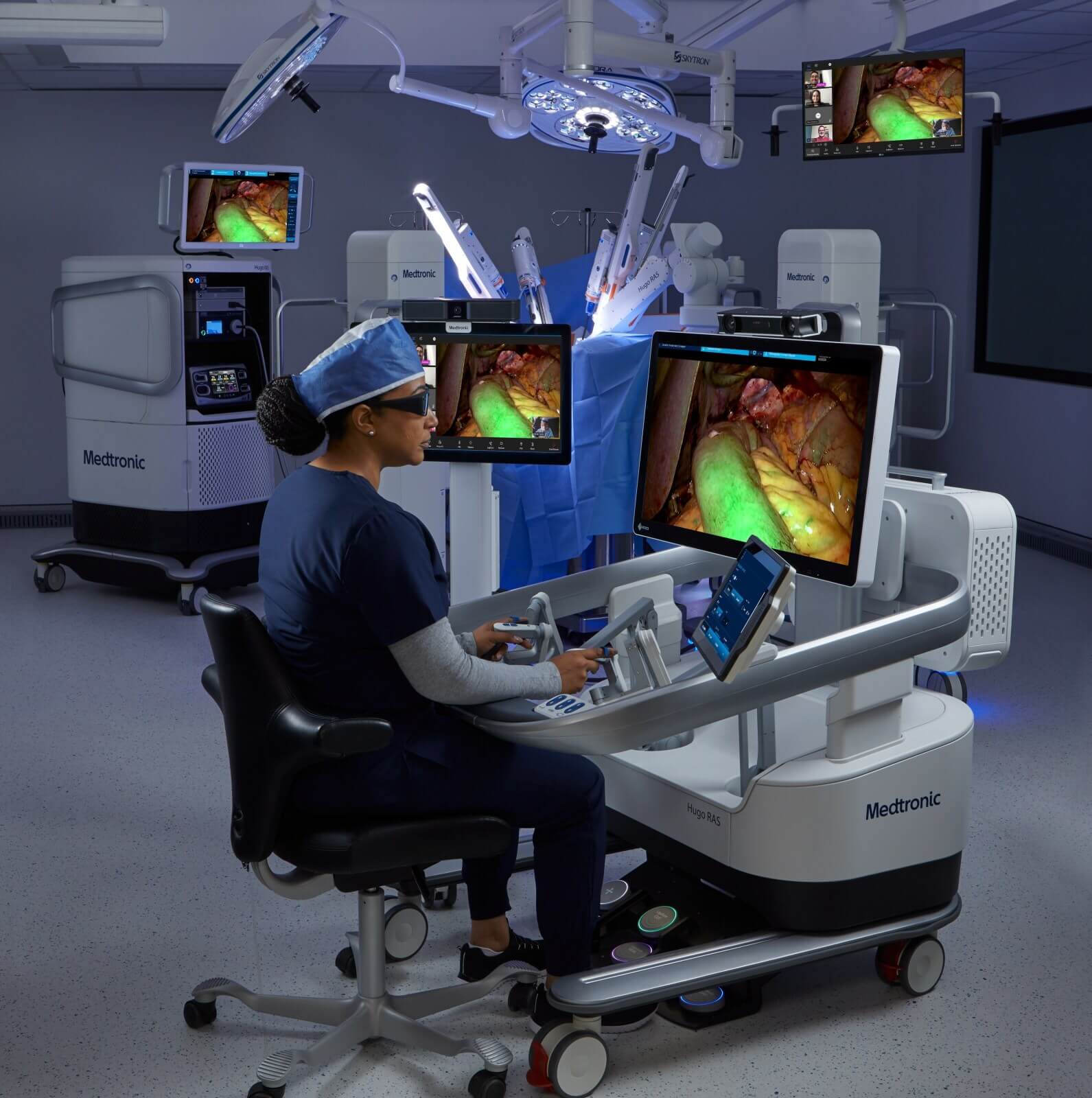
Medtronic Hugo RAS (US/global) — a soft‑tissue robotic system with telesurgical pilot studies underway; used in urologic and gynecologic operations and expanding to general surgery.
Asensus Senhance (US) — under active investigation for telesurgery and remote proctoring, applied in laparoscopic general and gynecologic surgery.
Virtual Incision MIRA (US) — a miniaturised robotic platform tested for remote telesurgical operation and NASA’s space‑based surgical experiments; used in colon resection and general surgery.
In July 2025, the World Health Organization and the Society of Robotic Surgery signed a formal agreement to advance equitable access to telesurgery globally, with a specific focus on low- and middle-income countries. The initiative includes plans for remote surgical mentoring, where experienced surgeons guide colleagues through complex procedures in real time, addressing training gaps as well as access gaps.
The barriers still to solve
Telesurgery is real and working. Scaling it is a different problem.
In many low-resource regions, the connectivity infrastructure simply is not there yet: long-distance telesurgery requires major investment in fiber optic networks, and any system needs robust backups because a dropped connection mid-procedure is not a theoretical risk.
Regulation is another bottleneck, since cross-border surgery raises unresolved questions about liability, licensing jurisdiction, and patient consent, all of which will determine whether hospitals and insurers permit telesurgery at scale.
Cybersecurity is equally central, because a surgical robot receiving real-time instructions over a network is a connected system, and standardized security protocols for telesurgery do not yet exist.
And then there is cost: even the newer, more affordable robotic platforms still represent significant capital outlay for hospitals in low-resource settings, and viable financing models have not been developed at meaningful scale.
Bottom line
Telesurgery has crossed from proof-of-concept into repeatable clinical practice. The technology works. The FDA has approved its first transcontinental trial. The WHO is treating it as a serious tool for global health equity.
What comes next depends less on the robots and more on the infrastructure, regulation, and financing that would allow this to scale. For healthcare leaders and investors, that's where the real opportunity and the real work sits.
Innovation highlights
❤️ Mammograms read your heart. Women already show up for mammograms – now those same scans could flag heart disease before it strikes. A study of 123,762 women, led by Emory University's Dr. Hari Trivedi, found that AI can detect calcium deposits in breast arteries from standard mammogram images. Women with severe calcification faced two to three times the cardiovascular risk. No extra tests, no extra cost – just a smarter use of a screening women already trust.
🧠 Lab brains get real home. Researchers have created ultralight 3D scaffolds – called aerohydrogels – that let human brain cells grow and communicate in conditions that closely mimic the real brain. Unlike conventional scaffolds that dissolve within days, these structures stay stable and allow precise control over stiffness and pore size. In lab tests, astrocytes and microglia not only survived but exchanged signals, with astrocytes visibly calming inflammatory responses in nearby immune cells.
🔬 AI spots cancer's escape plan. Some tumors stay put. Others spread – and until now, predicting which was guesswork. Researchers at the University of Geneva studied gene-expression patterns in colon cancer cells to understand what makes some tumors turn invasive. Their AI tool, MangroveGS, analyzes hundreds of gene signatures to predict metastatic risk with nearly 80% accuracy, outperforming existing tools. It works across multiple cancer types too, including stomach, lung, and breast. A simple tumor sample could one day generate a risk score sent directly to oncologists.
🏥 AI beats hospital bugs. Hospital-acquired infections like MRSA and C. difficile consume millions of excess NHS bed days each year – but up to 55% may be preventable with earlier detection. MEMORI, an AI-powered clinical decision support platform developed by Sanome and the NIHR Exeter HealthTech Research Centre, predicts infection risk up to seven days before symptoms appear. A new Innovate UK grant will boost its predictive accuracy by a further 20%, with trials now underway at Royal Devon University Healthcare NHS Foundation Trust.
Company to watch
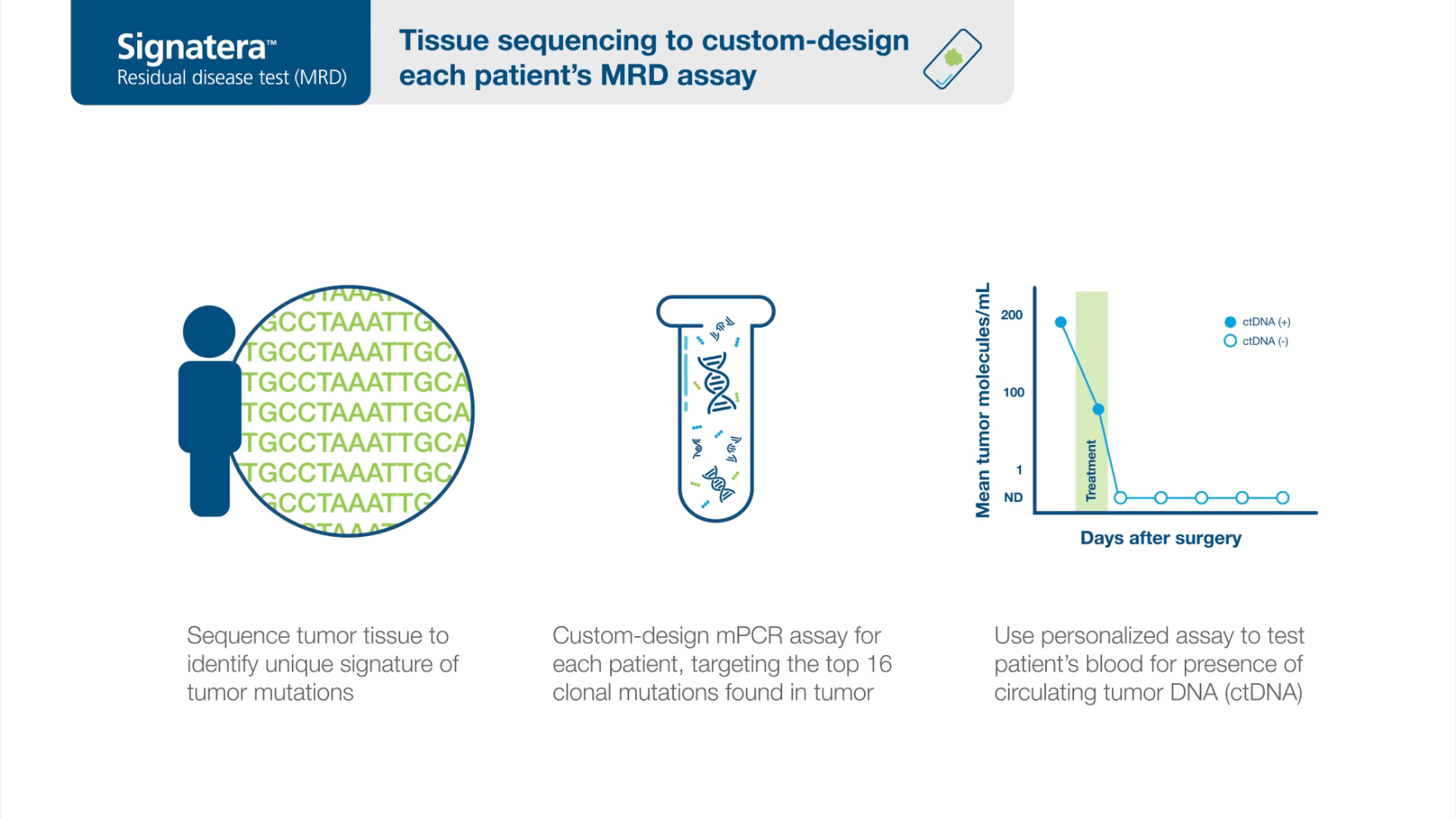
🧬 Natera is redefining how cancer is monitored and treated through cell-free DNA testing. Founded in 2004 and headquartered in Austin, Texas, the company's flagship Signatera test detects tiny traces of circulating tumor DNA in the blood, spotting cancer recurrence months before traditional imaging.
Signatera is personalized to each patient's unique tumor DNA, making it one of the more precise tools available for molecular residual disease detection across multiple cancer types. The December 2025 acquisition of Foresight Diagnostics expanded Natera's capabilities in lymphoma, a cancer affecting more than 75,000 Americans annually, adding Foresight's ultrasensitive PhasED-Seq technology to the Signatera platform.
Beyond oncology, Natera's testing portfolio covers women's health and organ transplant monitoring, positioning the company across three of medicine's most data-hungry specialties.
Weird and wonderful
🤜 Left hand, competitive edge. Left-handedness has puzzled evolutionary biologists for decades — if it were truly useful, shouldn't more of us have it? Researchers at the University of Chieti-Pescara in Italy studied over 1,100 people and found the answer hiding in competitive psychology. Left-handers scored significantly higher on "hypercompetitiveness" – an intense desire to win, even at others' expense – while right-handers gravitated toward cooperation.
The evolutionary logic: at roughly 10% of the population, left-handers are rare enough to stay unpredictable in one-on-one competition. Think boxing, tennis, that awkward first handshake. If southpaws became common, the advantage would disappear. Nature, it turns out, has been quietly running a minority strategy for thousands of years.

Image created using Canva AI
Thank you for reading the Healthy Innovations newsletter!
Keep an eye out for next week’s issue, where I will highlight the healthcare innovations you need to know about.
Have a great week!
Alison ✨
P.S. If you enjoyed reading the Healthy Innovations newsletter, please subscribe so I know the content is valuable to you!
P.P.S. Healthcare is evolving at an unprecedented pace, and your unique insights could be invaluable to others in the field. If you're considering starting your own newsletter to share your expertise and build a community around your healthcare niche, check out beehiiv (affiliate link). There's never been a better time to start sharing your knowledge with the world!